Why Are There So Few Black Men In Medicine?
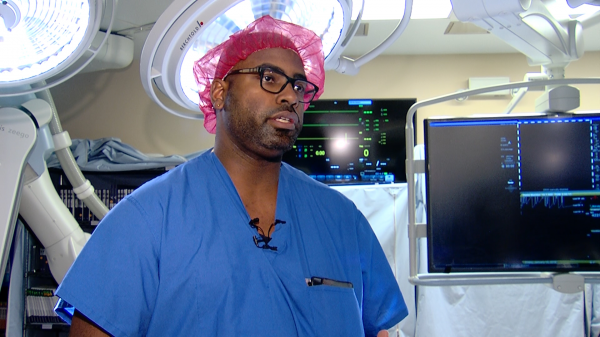
Dr. Don Arnold is chief of surgery at Herrin hospital and performs robotic surgery. Benjy Jeffords/WSIU
Dr. Don Arnold’s home office overflows with medical textbooks, old anatomical prints and six pages of a recommendation letter from his first application to medical school - framed and hanging on the wall.
“It says I have very unique and viable talents that would serve me well, but on paper a very poor academic record,” he says. “So this is code. For those who don’t know. Nobody’s going to outwardly tell you not to take a person, but this is how they write it in code.”

One page from the letter, which fills six frames.
Despite the less-than-stellar recommendation, Arnold, who is black, did eventually get into and graduate from medical school. Today, he is chief of surgery at Herrin Hospital, just outside of Carbondale, Illinois. Getting there wasn’t easy.
In 2018, fewer than 4 percent of incoming medical students in Illinois were black men. It’s a concerning statistic as research suggests a lack of diversity among physicians could negatively impact health outcomes in their community. The roots of this problem are deep. But medical schools and even health insurers in Illinois are taking steps to address the problem. Next month, a summit in Chicago will bring together medical providers to talk about improving physician diversity.
Educational Barriers Start Early
Arnold says the recommendation letter was far from the first challenge he faced while becoming a physician. During high school, his mother, frustrated with how quickly he finished his homework, suggested he enroll in advanced physics. The school at first said no - although they did eventually allow him in the course.
His story isn’t unique. African-American students are less likely to enroll in advanced classes than their white counterparts, especially math and science, which are critical for future medical careers. In Illinois, black students make up 17 percent of the student population - but just 7.8 percent of AP students.
On top of that, minority students tend to be concentrated in higher poverty areas. That means less funding for schools, which tend to be lower performing.
That’s something Jonathan Tyes, an aspiring medical school student, realized when he arrived at Morehouse College in Georgia. Tyes grew up in Ohio before attending the historically black college. He graduated from his public high school near the top of his class.
“Getting to undergrad at Morehouse, I realized how behind I really was,” he says. “Because I was competing with students who had been at private schools, and so they were testing into classes three classes past any math class I had to take.”

Jonathan Tyes holds a bear a friend gave him to remind him of his goals.
A Financial Stretch
Education isn’t the only hurdle to cross. There are financial hurdles as well. Simply applying to medical school costs thousands of dollars.
“It was hard for me to afford the testing at each level in this whole process, which is another reason I think you don’t see many African-Americans,” Arnold said. “You know, some of these exams, my mother wouldn’t pay bills so I would have money for the exams.”
The wealth gap in America is significant. As of 2016, African-American families had a median net worth of less than $18,000. Compare that to white families, whose median wealth came in at $171,000.
Arnold’s recommendation letter also noted that he faced financial challenges while in college, which could contribute to poor academic performance. Tyes, a first-generation college student, was also helping care for his nine younger siblings and aging grandparents.
Once enrolled, the average medical student graduates with nearly $200,000 in debt. Residency and fellowship applications cost additional money - all before a physician starts working.
In a highly competitive process where students often apply to 15 or more residency programs in hopes of getting in, Arnold was constrained by finances. He only applied to three.
“I had three interviews. I could only afford to go to two,” he says.

MEDPREP courses help students prepare to apply for medical school.
Creating Change
Tyes is involved in the MEDPREP program at Southern Illinois University Medical School. The post-college program helps academically disadvantaged students improve their performance before applying to medical school. Arnold attended a similar program in Chicago.
But programs like that can only serve a limited number of students.
Insurer Blue Cross Blue Shield is looking for other ways to increase diversity among physicians with a summit in Chicago in March. It will bring together medical schools, providers, and philanthropic organizations. One focus will be the pipeline to medical school that starts as early as elementary school.
Dr. Derek Robinson, chief medical officer for Blue Cross and Blue Shield of Illinois, acknowledges it’s an unusual topic for an insurer to address. But he says the costs of health disparities provide a business case for increasing physician diversity.
“This [is an] opportunity for us to help focus some attention on ensuring that we’re delivering a workforce that is best prepared to care for the growing, diverse population that we have both in the state and generally across the nation,” he says.
Addressing costs could also improve healthcare outcomes. Black men are more likely to suffer from chronic illness than their white counterparts. They’re more likely to die of heart disease or prostate cancer.
Research shows that black men are more likely to have preventative care done if their physician is also an African-American man. And that could reduce cardiovascular deaths.
It is, Robinson admits, a long-term goal and one that will take years to achieve.
But Arnold says students should have hope - he knows from experience that hard work and perseverance can go far.
“I’m nobody special. I didn’t come from it, it wasn’t given to me. I’m nobody but a person who had a dream and a person that persevered to achieve it,” he said.


