Champaign County Uninsured Rate Drops, But Not Everyone Pleased With Affordable Care Act

Champaign residents have seen a variety of effects from the Affordable Care Act. C-U Citizen Access
For Jim Bean, the Affordable Care Act meant hearing aids, new dentures, hernia surgery and the ability to go to the doctor on a regular basis.
For Loren Anderson, Obamacare meant “subsidizing the 86 percent of the people who can’t afford it” with $600 premiums and $13,000 deductibles.
For Chris Evans, the Affordable Care Act could have meant more time with his mother, Susan, who could have benefited from preventative health care and the medical tests needed to diagnose her lung cancer before it spread to her brain, eventually leading to her death.
These are just three of thousands of stories from people in Champaign County affected by the implementation of the Affordable Care Act.
These are just three of thousands of stories from people in Champaign County affected by the implementation of the Affordable Care Act.
On Thursday, the House of Representatives took the first step toward repealing and replacing the act. But as Congress continues to debate the future of health care, just what has the Affordable Care Act meant for people in Champaign County?
A look at the numbers:
- The uninsured rate in Champaign County dropped from 16 percent in 2013 to 5 percent in 2016, as more than 11,000 people gained health care, according to Enroll America.
- 6,891 people in Champaign County gained health insurance through the Medicaid expansion, according to the Illinois Department of Healthcare and Family Services.
- 4,336 people in Champaign enrolled in the federal health insurance marketplace, according the Center for Medicaid and Medicare Services.
- Promise Healthcare, a health care center that serves exclusively serves Medicaid and Medicare patients, has increased the number of people it serves from about 7,000 to 11,500, according to internal statistics.
Since its implementation in 2013, the act has expanded Medicaid coverage to cover more low-income people, allowed dependents to remain on their parents’ health insurance until 26 and prohibited insurers from denying coverage to people because of preexisting conditions.
The act also made sure insurance plans cover “Essential Health Benefits,” which are 10 categories that range from prescription drugs coverage — including birth control — to mental health services to emergency services. Additionally, the act mandated that every person must have insurance as a way to help keep prices down and also to encourage health coverage.
The Affordable Care Act gave Champaign County residents options that they didn’t have before 2013, said Claudia Lennhoff, the executive director of Champaign County Healthcare Consumers, a not-for-profit patient advocacy organization.
“Before the Affordable Care Act, so much of our client work focused on trying to help people with really impossible situations. It really felt like fishing bodies out of the river,” said Lennhoff, who said now the organization is able to proactively enroll people.
Yet the Affordable Care Act didn’t work for everyone. Many people saw premiums and deductibles rise. Undocumented immigrants, people who don’t enroll in Medicaid but are eligible and people who would rather pay the annual penalty or whose health insurance would cost more than 8 percent of their annual income still lack for health insurance.
Rep. Rodney Davis, a Republican who represents Champaign-Urbana as part of the 13th Congressional District, has led the fight to repeal and replace the Affordable Care Act.
Davis, who declined to be interviewed for this story via a spokeswoman, has argued that the Affordable Act has led to large increases in premiums and deductibles and resulted in fewer choices. His website says that millions of Americans can’t afford health insurance because of its high prices, and millions more can’t afford to use the insurance they have because of high deductibles.
Davis, who is a member of the moderate Tuesday Group, supported the American Health Care Act, though many of the group’s members did not. He also introduced a health care bill that he saw as part of a replacement for the Affordable Care Act.
“I want all Americans to have access to affordable health care but right now that’s not the case for many under Obamacare,” Davis said when he introduced the bill.
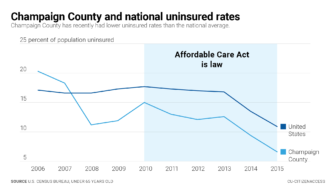
Champaign County and national uninsured rates have decreased with the ACA.
While he has pushed for a repeal of the Affordable Care Act, Davis, whose wife is a cancer survivor, said it is a priority for people with preexisting conditions to still have coverage. He has said it is important for people to make their own decisions about health care without government interference and the high costs that come along with the Affordable Care Act don’t allow people to make their own decisions.
Lennhoff said that Davis’ concerns about the act are misplaced.
“We can provide testament to the impact of the affordable care act and what it has done for people’s lives,” Lennhoff said. “And that is why I get so frustrated, for example, when we try to communicate with our legislators, our congressman, and he uses examples from his own life about why he does not support the affordable care act, and yet we have hundreds and thousands of examples that we can give that are the opposite, that shows that (the Affordable Care Act) has been working in the way that it was intended to work and has provided people with the health security they need so they can go on and live productive lives.”
Medicaid drives most growth in insurance enrollment
Because of the Medicaid expansion under the Affordable Care Act, 6,891 people in Champaign County gained health insurance.

Musician Jim Bean.
After being honorably discharged from the United States Navy in 1979, 57-year-old Champaign resident Jim Bean has been living without health insurance since. Aside from working as a musician, Bean worked various part-time jobs at the University of Illinois for more than 20 years, yet was never offered an insurance plan.
That is, however, until the expansion of Medicaid in 2013.
After enrolling in Medicaid, Bean was able to pay less for his dentures and his hernia surgery, hearing aids, physical therapy and regular doctor visits were covered.
Bean said he does enjoy the Affordable Care Act, but understands the issues it has, referring to the fact that adult vision care is not a required benefit.
“I am certainly aware that if they only repeal the act without replacing it with something very similar, then it’s probably going to have some negative effects on my life, and I guess we’ll just have to see one by one what those might be,” Bean said.
The expansion of Medicaid was passed in July 2013 and changed the requirements to apply.
More people now qualify for Medicaid, since the categorical requirements were reduced. People now only have to meet income guidelines, instead of being both low-income and fitting into another category, such as being pregnant, elderly, disabled or having children under 18 years old.
“Able-bodied childless low-income people used to not be able to qualify for Medicaid, but now under the expansion, they do,” said Claudia Lennhoff, the executive director of Champaign County Healthcare Consumers.
High premiums, deductibles drive residents to find alternatives
Loren Anderson, owner of the small Champaign business AFntronics, said he spent nine years attempting to find his least expensive option for health insurance.
Anderson’s wife was insured through her work, but the plan did not extend to him and their two children. Anderson eventually signed on with Humana and began paying $300 premiums and a deductible of about $6,500.

AFntronics owner Loren Anderson.
In September 2014, Anderson’s insurance provider cancelled his plan, saying they had to “conform to the act. ” He eventually enrolled in the Affordable Care Act and switched to Health Alliance as a provider.
“I was pretty excited about Obamacare,” Anderson said. “I heard a lot of good things.”
However, Anderson soon became discontented with his plan, as his premiums doubled to $600 a month and his deductible rose to $13,000.
“I tried Obamacare and it more than doubled my premium and because of my income, I got no subsidy, no discount whatsoever. I had to pay the full amount,” Anderson said. “I’m subsidizing the 86 percent of the people who can’t afford it. I just don’t see how that can be called the Affordable [Care] Act.”
Currently, Blue Cross Blue Shield is the only insurance company offering new plans through the marketplace in Champaign County after Health Alliance dropped out because of high costs.
Low-income and young people benefit the most from the act, while the American Health Care Act would lower out-of-pocket costs for many higher income people, the Kaiser Family Foundation found.
For example:
– For a 27-year-old with an annual income of $40,000, premiums would drop from an out-of-pocket cost of $4,080 to $2,260.
– For a 40-year-old with an annual income of $40,000, premiums would drop from an out-of-pocket cost of $4,080 to $2,630.
– For a 60-year-old with an annual income of $40,000, premiums would rise from an out-of-pocket cost of $4,080 to $12,070
Promise Healthcare sees boost in patients after Affordable Care Act
Promise Healthcare is a federally qualified health center, meaning it serves an underserved population. Its centers in Champaign, which include Frances Nelson health center, has had an uptake in clients who have health care in the last seven years, said Nancy Greenwalt, executive director.

Nancy Greenwalt, executive director of Promise Healthcare.
Before the implementation of the Affordable Care Act, 40 to 50 percent of patients did not have health insurance, Greenwalt said. By 2017, that number dropped to 20 percent of patients.
“After implementation, we worked really hard to get patients covered,” Greenwalt said.
Promise Healthcare expanded their efforts by adding staff members and focusing on outreach and enrollment, said Greenwalt. If a low-income, uninsured patient comes in, Promise Healthcare will treat the patient and then provide them with the resources necessary to enroll in Medicaid.
In 2013, Promise Healthcare served 7,041 patients, Greenwalt said. By 2016, it was 11,449.
“Health care is always changing,” Greenwalt said. “Hopefully we’re changing in ways that increase access to care and coverage.”
However, not all hospitals in Champaign County have seen positive increases.
Six percent more of the Carle Foundation Hospital’s clients were covered under Medicaid in 2016 than in 2010, said Jennifer Hendricks Kaufmann, public relations manager of the Carle Foundation, in an email.
“The percentage of uninsured or self-pay patients has not decreased significantly, staying at about the same level as in 2010,” Kaufmann said. In addition, the amounts of patients seeking charity care has not decreased since the implementation of the Affordable Care Act.
Presence Medical Center did not respond to requests for comment.
Repeal of Affordable Care Act leaves residents worried about side effects
Both proponents and opponents agree: There is little doubt that the Affordable Care Act is in jeopardy.
President Donald Trump spent a majority of his presidential campaign calling for a complete repeal and replace of the act. On Thursday, the House of Representatives passed the American Health Care Act, a start at repealing and replacing the Affordable Care Act that now moves on to the Senate.

Urbana resident Chris Evans is nervous about the health care system going backwards.
But what Urbana resident Chris Evans is currently worried about is going back to a time when the health care system did not work for people like his mother, Susan.
Susan, who did not qualify for Medicaid, avoided routine health care in fear of medical bills she would not be able to pay for.
But in 2008 she began to have occasional falls. Brushing them off as old age, Susan continued to forgo health care.
It was not until a year later that she called Chris after hitting her eye during a fall, and she suggested she finally go to the hospital.
“We took her in that May of 2009 to have her eye looked at and the doctor, within an hour, came back and told her she had stage four lung cancer and that it had metastasized to her brain and she had over 10 tumors in her brain,” Chris said. “She died about a month later.”
“We have a lot of clients who have gotten health insurance through the Medicaid expansion piece of the Affordable Care Act, and that under the Republican plan would end at the end of 2019,” said Claudia Lennhoff, executive director of Champaign County Healthcare Consumers.
Under the initial American Health Care Act, people who had been able to enroll in Medicaid due to the expansion would not immediately lose their insurance. However, the program would start to revert back to its pre-expansion coverage after 2020 and cease funding for states that want to enroll more people.
Illinois is one of eight states that have a “trigger” law, meaning any decreases in federal funding would cause an immediate redaction of the Medicaid expansion.
“There are a lot of people, especially in this community, who work low wage jobs that don’t offer health insurance, and who would actually qualify for Medicaid,” Lennhoff said. “I think one of the most devastating consequences of the Republican health care bill is not even what it does to the Affordable Care Act, but what it does to the long-standing Medicaid program.”
Links
- House Passes GOP Health Care Bill
- As House GOP Struggles With A Health Care Bill, Republican Options Narrow
- Republicans Kill Health Care Vote As GOP Members Defect
- Congressional Healthcare Bill Response Tracker
- Durbin Meets With Rockford-Area Healthcare Leaders About Repeal Plan
- Rauner: Illinois ‘Won’t Do Well’ Under House GOP Health Plan
- The Future Of The Nation’s Health Care Law

